Pancreatitis is a health condition in which the pancreas develops inflammation or infection (chronic pancreatitis).

Pancreatitis causes serious damage to the body’s organs and can be fatal.
Pancreatitis usually occurs due to some type of sudden onset of inflammation in the pancreas. Usually, acute pancreatitis is an inflammatory condition in which the pancreas gets inflamed (swelled) in a relatively short period of time.

Most patients with acute pancreatitis begin to feel more active within a few days and normally have no more problems.
In some cases, acute pancreatitis symptoms may be confused with symptoms that are indicative of pancreatic cancer. Although the symptoms of acute pancreatitis mimic those of pancreatic cancer, the two are quite different and usually go away on their own.
The most common acute pancreatitis symptoms include loss of appetite, nausea, vomiting and/or loss of weight. Patients also experience jaundice, dark urine and blood.
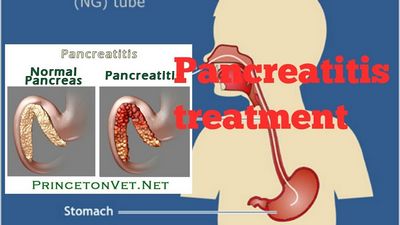
Since the symptoms of acute pancreatitis can be confused with pancreatic cancer, some physicians will refer patients for pancreatic biopsy as a precaution.
However, pancreatitis symptoms can often be mistaken for the signs of pancreatic cancer. Patients can get false alarms and treatments could not prove to be effective.
Because pancreatitis attacks the pancreas through the use of pancreatic enzymes, it is often called “enteric pancreatitis”. Some patients with pancreatitis will also exhibit signs of gallstones or kidney stones.
Because pancreatitis attacks the digestive tract, pancreatitis patients frequently exhibit abdominal pain, diarrhea and abdominal distention.
There may also be symptoms of cholestasis in the digestive system. A patient who has pancreatitis may also show evidence of jaundice (yellowing of the skin or eyes. In the liver, a patient may exhibit increased liver enzymes and bilirubin.
Leave a Reply